Advances in peptide-drug conjugates
Background
Cancer-related diseases have become the greatest menace to mortal health in the world, and it is an enormous challenge to ameliorate the treatment indicators of medication. It has always been the goal of many research groups to develop new therapies that are less harmful to patients. The prodrug is a temporary chemical combination or covering. After entering the body, it can be degraded according to the microenvironment in the body, releasing the original drug and exerting its own curative effect. The drug molecule can be combined with some small molecular substances that can change the biological activity of the drug to product a prodrug, which can effectively alteration the physical and chemical properties and biological properties of the drug to achieve the purpose of specific administration, this strategy can prevent the drug from being released prematurely, and has the advantages of promoting drug absorption, prolonging the action time, and improving targeting. In recent years, among many design strategies related to prodrugs, peptide-drug conjugates (PDCs) have attracted wide attention from researchers.
What is Peptide-drug Conjugates?
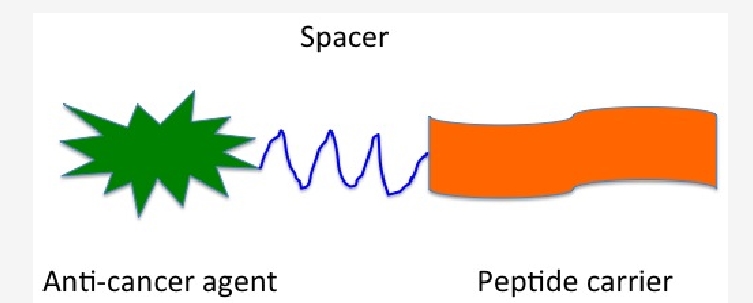
Peptide-drug conjugates are a new type of conjugated drug, which usually refers to the combination of drug and targeted peptide through appropriate conjugating agent. Once the conjugate enters cancer cells through receptor-mediated endocytosis, it will promote the chemical or enzymatic release of drug. By controlling the peptide chain of about 10 amino acid sequences, it can change its conjugated hydrophobicity and ionize and target tumor cells, which affect the bioavailability in vitro and in vivo, and without causing immune response. PDCs with low molecular weight can be easily purified by HPLC technology. These characteristics of PDCs are essential for optimizing pharmacokinetics. Peptide-drug conjugates are mainly composed of three parts: drug, polypeptide sequence with specific functions and degradable linkages. PDCs which through the carefully designed not only retains the advantages of traditional drug delivery, but also increases the penetration of tumor drugs and reduces the toxicity to liver and kidney. Many studies have confirmed that peptide conjugates provide a valuable substitute for anticancer drugs currently used for different types of cancers. The research study on PDCs at domestic and international mainly focuses on the structure and optimization design of peptide-drug conjugates, the methods of improving peptidase and chemical stability, the effect of targeted therapy on the specificity of tumor cells, the internalization mechanism of PDCs in vivo, and so on. With the extensive development of basic research study, the scope of clinical application research on PDCs has gradually expanded, and rational use of the biological mechanism of peptide action can effectively treat a variety of diseases.
Application of Peptide-drug Conjugates
The application of peptide-drug conjugates in the treatment of cancer is a relatively new field. At present, several peptide-drug conjugates have been developed, and some of these efforts have been clinically scored. Peptide-drug conjugates have the advantages of no hematological or other toxicity, high stability and tissue specificity, and have broad application prospects in the field of anti-cancer therapy. However, most of the nano-drugs constructed by peptide-drug conjugates have a single function at present, and the in vivo environment of organisms is very complex, so the effectiveness of crossing multiple biological barriers needs to be improved. It is the primary task to design polypeptide-drug conjugates with strong compatibility, such as targeting function and stealth function, so that drugs can effectively cross multiple barriers of the body, act on targets, improve the effective therapeutic concentration of drugs, and exert curative effect. Therefore, peptide-drug conjugates still have many fields need to be explored. It can be predicted that the successful transition from laboratory to clinic is only a matter of time, while the transition from laboratory to clinic is time-consuming. The recent progress should promote this transition, lay a foundation for the great progress of PDCs targeted treatment of cancer, and also provide a new strategy for promoting the active monomer of traditional Chinese medicine to enter the clinic.
Frequently Asked Questions (FAQ)
Conjugation efficiency can be improved by adjusting reaction conditions, optimizing molar ratios, and using high-precision coupling reagents to ensure uniform product formation.
Peptide chain length affects molecular flexibility, receptor binding, and solubility, which together influence overall delivery and stability.
The linker controls how and when the two components interact or separate, influencing both functional stability and targeted release.
Scalability depends on reaction yield, purification throughput, and compatibility of lab-scale chemistry with larger reactor systems.


References:
- Chari, R. V., Miller, M. L., & Widdison, W. C. (2014). Antibody–drug conjugates: an emerging concept in cancer therapy. Angewandte Chemie International Edition, 53(15), 3796-3827.
- Su, H., Koo, J. M., & Cui, H. (2015). One-component nanomedicine. Journal of controlled release, 219, 383-395.
- Majumdar, S., & Siahaan, T. J. (2012). Peptide‐mediated targeted drug delivery. Medicinal research reviews, 32(3), 637-658.
- Hawryłkiewicz, A., & Ptaszyńska, N. (2021). Gemcitabine Peptide-Based Conjugates and Their Application in Targeted Tumor Therapy. Molecules, 26(2), 364.
- Cooper, B. M., Iegre, J., O'Donovan, D. H., Halvarsson, M. Ö., & Spring, D. R. (2021). Peptides as a platform for targeted therapeutics for cancer: peptide–drug conjugates (PDCs). Chemical Society Reviews.
- Sun, L., & Coy, D. H. (2014). Anti-convulsant drug valproic acid in cancers and in combination anti-cancer therapeutics. Mod Chem Appl, 2(1), 1-5.